Swine influenza (also called swine flu, hog flu, and pig flu) refers to influenza caused by those strains of influenza virus, called swine influenza virus (SIV), that usually infect pigs. Swine influenza is common in pigs in the midwestern United States (and occasionally in other states), Mexico, Canada, South America, Europe (including the United Kingdom, Sweden, and Italy), Kenya, Mainland China, Taiwan, Japan and other parts of eastern Asia.
Transmission of swine influenza virus from pigs to humans is not common and properly cooked pork poses no risk of infection. When transmitted, the virus does not always cause human influenza and often the only sign of infection is the presence of antibodies in the blood, detectable only by laboratory tests. When transmission results in influenza in a human, it is called zoonotic swine flu. People who work with pigs, especially people with intense exposures, are at risk of catching swine flu. However, only about fifty such transmissions have been recorded since the mid-20th Century, when identification of influenza subtypes became possible. Rarely, these strains of swine flu can pass from human to human. In humans, the symptoms of swine flu are similar to those of influenza and of influenza-like illness in general, namely chills, fever, sore throat, muscle pains, severe headache, coughing, weakness and general discomfort.
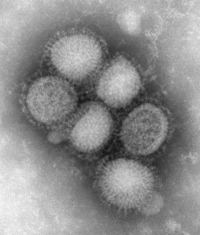
The 2009 flu outbreak in humans, known as "swine flu", is due to a new strain of influenza A virus subtype H1N1 that contained genes most closely related to swine influenza. The origin of this new strain is unknown, however, the World Organization for Animal Health (OIE) reports that this strain has not been isolated in pigs. This strain can be transmitted from human to human, and causes the normal symptoms of influenza.
Classification
Of the three genera of influenza viruses that cause human flu, two also cause influenza in pigs, with Influenzavirus A being common in pigs and Influenzavirus C being rare. Influenzavirus B has not been reported in pigs. Within Influenzavirus A and Influenzavirus C, the strains found in pigs and humans are largely distinct, although due to reassortment there have been transfers of genes among strains crossing swine, avian, and human species boundaries.
Influenza C
Influenza C viruses infect both humans and pigs, but do not infect birds. Transmission between pigs and humans have occurred in the past. For example, influenza C caused a small outbreaks of a mild form of influenza amongst children in Japan, and California. Due to its limited host range and the lack of genetic diversity in influenza C, this form of influenza does not cause pandemics in humans.
Influenza A
Swine influenza is known to be caused by influenza A subtypes H1N1, H1N2, H3N1, H3N2, and H2N3. In pigs, three influenza A virus subtypes (H1N1, H3N2, and H1N2) are the most common strains worldwide. In the United States, the H1N1 subtype was exclusively prevalent among swine populations before 1998; however, since late August 1998, H3N2 subtypes have been isolated from pigs. As of 2004, H3N2 virus isolates in US swine and turkey stocks were triple reassortants, containing genes from human (HA, NA, and PB1), swine (NS, NP, and M), and avian (PB2 and PA) lineages.
Surveillance
| Please help improve this article or section by expanding it. Further information might be found on the talk page. (May 2009) |
Although there is no formal national surveillance system in the United States to determine what viruses are circulating in pigs, there is an informal surveillance network in the United States that is part of a world surveillance network.
History
Swine influenza was first proposed to be a disease related to human influenza during the 1918 flu pandemic, when pigs became sick at the same time as humans. The first identification of an influenza virus as a cause of disease in pigs occurred about ten years later, in 1930. For the following 60 years, swine influenza strains were almost exclusively H1N1. Then, between 1997 and 2002, new strains of three different subtypes and five different genotypes emerged as causes of influenza among pigs in North America. In 1997-1998, H3N2 strains emerged. These strains, which include genes derived by reassortment from human, swine and avian viruses, have become a major cause of swine influenza in North America. Reassortment between H1N1 and H3N2 produced H1N2. In 1999 in Canada, a strain of H4N6 crossed the species barrier from birds to pigs, but was contained on a single farm.
The H1N1 form of swine flu is one of the descendants of the strain that caused the 1918 flu pandemic. As well as persisting in pigs, the descendants of the 1918 virus have also circulated in humans through the 20th century, contributing to the normal seasonal epidemics of influenza. However, direct transmission from pigs to humans is rare, with only 12 cases in the U.S. since 2005. Nevertheless, the retention of influenza strains in pigs after these strains have disappeared from the human population might make pigs a reservoir where influenza viruses could persist, later emerging to reinfect humans once human immunity to these strains has waned.
Swine flu has been reported numerous times as a zoonosis in humans, usually with limited distribution, rarely with a widespread distribution. Outbreaks in swine are common and cause significant economic losses in industry, primarily by causing stunting and extended time to market. For example, this disease costs the British meat industry about £65 million pounds every year.
1918 pandemic in humans
The 1918 flu pandemic in humans was associated with H1N1 and influenza appearing in pigs, thus may reflect a zoonosis either from swine to humans, or from humans to swine. Although it is not certain in which direction the virus was transferred, some evidence suggests that, in this case, pigs caught the disease from humans. For instance, swine influenza was only noted as a new disease of pigs in 1918, after the first large outbreaks of influenza amongst people. Although a recent phylogenetic analysis of more recent strains of influenza in humans, birds, and swine suggests that the 1918 outbreak in humans followed a reassortment event within a mammal, the exact origin of the 1918 strain remains elusive.
1976 U.S. outbreak
On February 5, 1976, in the United States an army recruit at Fort Dix said he felt tired and weak. He died the next day and four of his fellow soldiers were later hospitalized. Two weeks after his death, health officials announced that the cause of death was a new strain of swine flu. The strain, a variant of H1N1, is known as A/New Jersey/1976 (H1N1). It was detected only from January 19 to February 9 and did not spread beyond Fort Dix.
This new strain appeared to be closely related to the strain involved in the 1918 flu pandemic. Moreover, the ensuing increased surveillance uncovered another strain in circulation in the U.S.: A/Victoria/75 (H3N2) spread simultaneously, also caused illness, and persisted until March. Alarmed public-health officials decided action must be taken to head off another major pandemic, and urged President Gerald Ford that every person in the U.S. be vaccinated for the disease.
The vaccination program was plagued by delays and public relations problems. On October 1, 1976, the immunization program began and by October 11, approximately 40 million people, or about 24% of the population, had received swine flu immunizations. That same day, three senior citizens died soon after receiving their swine flu shots and there was a media outcry linking the deaths to the immunizations, despite the lack of positive proof. According to science writer Patrick Di Justo, however, by the time the truth was known — that the deaths were not proven to be related to the vaccine — it was too late. "The government had long feared mass panic about swine flu — now they feared mass panic about the swine flu vaccinations." This became a strong setback to the program.
There were reports of Guillain-Barré syndrome, a paralyzing neuromuscular disorder, affecting some people who had received swine flu immunizations. This syndrome is a rare side-effect of modern influenza vaccines, with an incidence of about one case per million vaccinations. As a result, Di Justo writes that "the public refused to trust a government-operated health program that killed old people and crippled young people." In total, less than 33 percent of the population had been immunized by the end of 1976. The National Influenza Immunization Program was effectively halted on Dec. 16.
Overall, about 500 cases of Guillain-Barré syndrome (GBS), resulting in death from severe pulmonary complications for 25 people, which, according to Dr. P. Haber, were probably caused by an immunopathological reaction to the 1976 vaccine. Other influenza vaccines have not been linked to GBS, though caution is advised for certain individuals, particularly those with a history of GBS. Still, as observed by a participant in the immunization program, the vaccine killed more Americans than the disease did.
1988 zoonosis
In September 1988, a swine flu virus killed one woman in Wisconsin, and infected at least hundreds of others. 32-year old Barbara Ann Wieners was eight months pregnant when she and her husband, Ed, became ill after visiting the hog barn at the Walworth County Fair. Barbara died eight days later, though doctors were able to induce labor and deliver a healthy daughter before she passed away. Her husband recovered from his symptoms.
Influenza-like illnesses were reportedly widespread among the pigs at the farm they had visited, and 76% of the swine exhibitors there tested positive for antibody to SIV, but no serious illnesses were detected among this group. Additional studies suggested between one and three health care personnel who had contact with the patient developed mild influenza-like illnesses with antibody evidence of swine flu infection. However, there was no community outbreak.
1998 US outbreak in swine
In 1998, swine flu was found in pigs in four U.S. states. Within a year, it had spread through pig populations across the United States. Scientists found that this virus had originated in pigs as a recombinant form of flu strains from birds and humans. This outbreak confirmed that pigs can serve as a crucible where novel influenza viruses emerge as a result of the reassortment of genes from different strains.
2007 Philippine outbreak in swine
| Please help improve this article or section by expanding it. Further information might be found on the talk page. (April 2009) |
On August 20, 2007 Department of Agriculture officers investigated the outbreak (epizootic) of swine flu in Nueva Ecija and Central Luzon, Philippines. The mortality rate is less than 10% for swine flu, unless there are complications like hog cholera. On July 27, 2007, the Philippine National Meat Inspection Service (NMIS) raised a hog cholera "red alert" warning over Metro Manila and 5 regions of Luzon after the disease spread to backyard pig farms in Bulacan and Pampanga, even if these tested negative for the swine flu virus.
2009 outbreak in humans
The 2009 flu outbreak is due to a new strain of subtype H1N1 not previously reported in pigs.[41] Following the outbreak, on May 2, 2009, it was reported in pigs at a farm in Alberta, Canada, with a link to the outbreak in Mexico. The pigs are suspected to have caught this new strain of virus from a farm worker who recently returned from Mexico, then showed symptoms of an influenza-like illness. These are probable cases, pending confirmation by laboratory testing.
The new strain was initially described as apparent reassortment of at least four strains of influenza A virus subtype H1N1, including one strain endemic in humans, one endemic in birds, and two endemic in swine. Subsequent analysis suggested it was a reassortment of just two strains, both found in swine. Although initial reports identified the new strain as swine influenza (ie, a zoonosis originating in swine), its origin is unknown. Several countries took precautionary measures to reduce the chances for a global pandemic of the disease.
Transmission
Transmission between pigs
Influenza is quite common in pigs, with about half of breeding pigs having been exposed to the virus in the US. Antibodies to the virus are also common in pigs in other countries.
The main route of transmission is through direct contact between infected and uninfected animals. These close contacts are particularly common during animal transport. Intensive farming may also increase the risk of transmission, as the pigs are raised in very close proximity to each other. The direct transfer of the virus probably occurs either by pigs touching noses, or through dried mucus. Airborne transmission through the aerosols produced by pigs coughing or sneezing are also an important means of infection. The virus usually spreads quickly through a herd, infecting all the pigs within just a few days. Transmission may also occur through wild animals, such as wild boar, which can spread the disease between farms.
Transmission to humans
People who work with poultry and swine, especially people with intense exposures, are at increased risk of zoonotic infection with influenza virus endemic in these animals, and constitute a population of human hosts in which zoonosis and reassortment can co-occur. Vaccination of these workers against influenza and surveillance for new influenza strains among this population may therefore be a important public health measure. Transmission of influenza from swine to humans who work with swine was documented in a small surveillance study performed in 2004 at the University of Iowa. This study among others forms the basis of a recommendation that people whose jobs involve handling poultry and swine be the focus of increased public health surveillance. Other professions at particular risk of infection are veterinarians and meat processing workers, although the risk of infection for both of these groups is lower than that of farm workers.
Interaction with avian H5N1 in pigs
Pigs are unusual as they can be infected with influenza strains that usually infect three different species: pigs, birds and humans. This makes pigs a host where influenza viruses might exchange genes, producing new and dangerous strains. Avian influenza virus H3N2 is endemic in pigs in China and has been detected in pigs in Vietnam, increasing fears of the emergence of new variant strains. H3N2 evolved from H2N2 by antigenic shift. In August 2004, researchers in China found H5N1 in pigs.

Signs and symptoms
In swine
In pigs influenza infection produces fever, lethargy, sneezing, coughing, difficulty breathing and decreased appetite. In some cases the infection can cause abortion. Although mortality is usually low (around 1-4%), the virus can produce weight loss and poor growth, causing economic loss to farmers. Infected pigs can lose up to 12 pounds of body weight over a 3 to 4 week period.
In humans
Direct transmission of a swine flu virus from pigs to humans is occasionally possible (called zoonotic swine flu). In all, 50 cases are known to have occurred since the first report in medical literature in 1958, which have resulted in a total of six deaths. Of these six people, one was pregnant, one had leukemia, one had Hodgkin disease and two were known to be previously healthy. Despite these apparently low numbers of infections, the true rate of infection may be higher, since most cases only cause a very mild disease, and will probably never be reported or diagnosed.
According to the Centers for Disease Control and Prevention (CDC), in humans the symptoms of the 2009 "swine flu" H1N1 virus are similar to those of influenza and of influenza-like illness in general. Symptoms include fever, cough, sore throat, body aches, headache, chills and fatigue. The 2009 outbreak has shown an increased percentage of patients reporting diarrhea and vomiting. The 2009 H1N1 virus is not zoonotic swine flu, as it is not transmitted from pigs to humans, but from person to person.
Because these symptoms are not specific to swine flu, a differential diagnosis of probable swine flu requires not only symptoms but also a high likelihood of swine flu due to the person's recent history. For example, during the 2009 swine flu outbreak in the United States, CDC advised physicians to "consider swine influenza infection in the differential diagnosis of patients with acute febrile respiratory illness who have either been in contact with persons with confirmed swine flu, or who were in one of the five U.S. states that have reported swine flu cases or in Mexico during the 7 days preceding their illness onset." A diagnosis of confirmed swine flu requires laboratory testing of a respiratory sample (a simple nose and throat swab).
Prevention
Prevention of swine influenza has three components: prevention in swine, prevention of transmission to humans, and prevention of its spread among humans.
Prevention in swine
Methods of preventing the spread of influenza among swine include facility management, herd management, and vaccination. Because much of the illness and death associated with swine flu involves secondary infection by other pathogens, control strategies that rely on vaccination may be insufficient.
Control of swine influenza by vaccination has become more difficult in recent decades, as the evolution of the virus has resulted in inconsistent responses to traditional vaccines. Standard commercial swine flu vaccines are effective in controlling the infection when the virus strains match enough to have significant cross-protection, and custom (autogenous) vaccines made from the specific viruses isolated are created and used in the more difficult cases. Present vaccination strategies for SIV control and prevention in swine farms typically include the use of one of several bivalent SIV vaccines commercially available in the United States. Of the 97 recent H3N2 isolates examined, only 41 isolates had strong serologic cross-reactions with antiserum to three commercial SIV vaccines. Since the protective ability of influenza vaccines depends primarily on the closeness of the match between the vaccine virus and the epidemic virus, the presence of nonreactive H3N2 SIV variants suggests that current commercial vaccines might not effectively protect pigs from infection with a majority of H3N2 viruses. The United States Department of Agriculture researchers say that while pig vaccination keeps pigs from getting sick, it does not block infection or shedding of the virus.
Facility management includes using disinfectants and ambient temperature to control virus in the environment. The virus is unlikely to survive outside living cells for more than two weeks, except in cold (but above freezing) conditions, and it is readily inactivated by disinfectants. Herd management includes not adding pigs carrying influenza to herds that have not been exposed to the virus. The virus survives in healthy carrier pigs for up to 3 months and can be recovered from them between outbreaks. Carrier pigs are usually responsible for the introduction of SIV into previously uninfected herds and countries, so new animals should be quarantined. After an outbreak, as immunity in exposed pigs wanes, new outbreaks of the same strain can occur.
Prevention in humans
- Prevention of pig to human transmission

The transmission from swine to human is believed to occur mainly in swine farms where farmers are in close contact with live pigs. Although strains of swine influenza are usually not able to infect humans this may occasionally happen, so farmers and veterinarians are encouraged to use a face mask when dealing with infected animals. The use of vaccines on swine to prevent their infection is a major method of limiting swine to human transmission. Risk factors that may contribute to swine-to-human transmission include smoking and not wearing gloves when working with sick animals.
- Prevention of human to human transmission
Influenza spreads between humans through coughing or sneezing and people touching something with the virus on it and then touching their own nose or mouth. Swine flu cannot be spread by pork products, since the virus is not transmitted through food. The swine flu in humans is most contagious during the first five days of the illness although some people, most commonly children, can remain contagious for up to ten days. Diagnosis can be made by sending a specimen, collected during the first five days for analysis.
Recommendations to prevent spread of the virus among humans include using standard infection control against influenza. This includes frequent washing of hands with soap and water or with alcohol-based hand sanitizers, especially after being out in public. Although the current trivalent influenza vaccine is unlikely to provide protection against the new 2009 H1N1 strain, vaccines against the new strain are being developed and could be ready as early as June 2009.
Experts agree that hand-washing can help prevent viral infections, including ordinary influenza and the swine flu virus. Influenza can spread in coughs or sneezes, but an increasing body of evidence shows small droplets containing the virus can linger on tabletops, telephones and other surfaces and be transferred via the fingers to the mouth, nose or eyes. Alcohol-based gel or foam hand sanitizers work well to destroy viruses and bacteria. Anyone with flu-like symptoms such as a sudden fever, cough or muscle aches should stay away from work or public transportation and should contact a doctor to be tested.
Social distancing is another tactic. It means staying away from other people who might be infected and can include avoiding large gatherings, spreading out a little at work, or perhaps staying home and lying low if an infection is spreading in a community. Public health and other responsible authorities have action plans which may request or require social distancing actions depending on the severity of the outbreak.
Treatment
In swine
As swine influenza is rarely fatal to pigs, little treatment beyond rest and supportive care is required. Instead veterinary efforts are focused on preventing the spread of the virus throughout the farm, or to other farms. Vaccination and animal management techniques are most important in these efforts. Antibiotics are also used to treat this disease, which although they have no effect against the influenza virus, do help prevent bacterial pneumonia and other secondary infections in influenza-weakened herds.
In humans
If a person becomes sick with swine flu, antiviral drugs can make the illness milder and make the patient feel better faster. They may also prevent serious flu complications. For treatment, antiviral drugs work best if started soon after getting sick (within 2 days of symptoms). Beside antivirals, palliative care, at home or in hospital, focuses on controlling fevers and maintaining fluid balance. The U.S. Centers for Disease Control and Prevention recommends the use of Tamiflu (oseltamivir) or Relenza (zanamivir) for the treatment and/or prevention of infection with swine influenza viruses, however, the majority of people infected with the virus make a full recovery without requiring medical attention or antiviral drugs. The virus isolates in the 2009 outbreak have been found resistant to amantadine and rimantadine.
In the U.S., on April 27, 2009, the FDA issued Emergency Use Authorizations to make available Relenza and Tamiflu antiviral drugs to treat the swine influenza virus in cases for which they are currently unapproved. The agency issued these EUAs to allow treatment of patients younger than the current approval allows and to allow the widespread distribution of the drugs, including by non-licensed volunteers.
%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%%








0 comments:
Post a Comment